Overview
Nobody thinks about hospital networks until they're standing at a reception desk, policy card in hand, being told the hospital is not covered. At that point, you have two options: pay the full bill upfront or leave and find another hospital. Neither is a good situation to be in.
This is where the Tata AIG health insurance network hospital list helps. A network hospital settles eligible bills directly with the insurer, so you walk out without worrying about arranging funds or waiting weeks for a reimbursement to come through.
Free Tata AIG Network Hospital List PDF Download
We've compiled the full Tata AIG network hospital list into a downloadable PDF for your convenience. You can find it below:
Note: Tata AIG health insurance has more than 11,000 network hospitals nationwide, exceeding our recommended benchmark of 10,000+. So, whether you live in a metro city or a smaller town, chances are you have a network hospital near you.
How to Find Tata AIG Network Hospital List Online
The most accurate and up-to-date source is the official Tata AIG hospital locator. Enter your city, and the tool will show all empaneled hospitals in your area, along with their addresses and contact details.
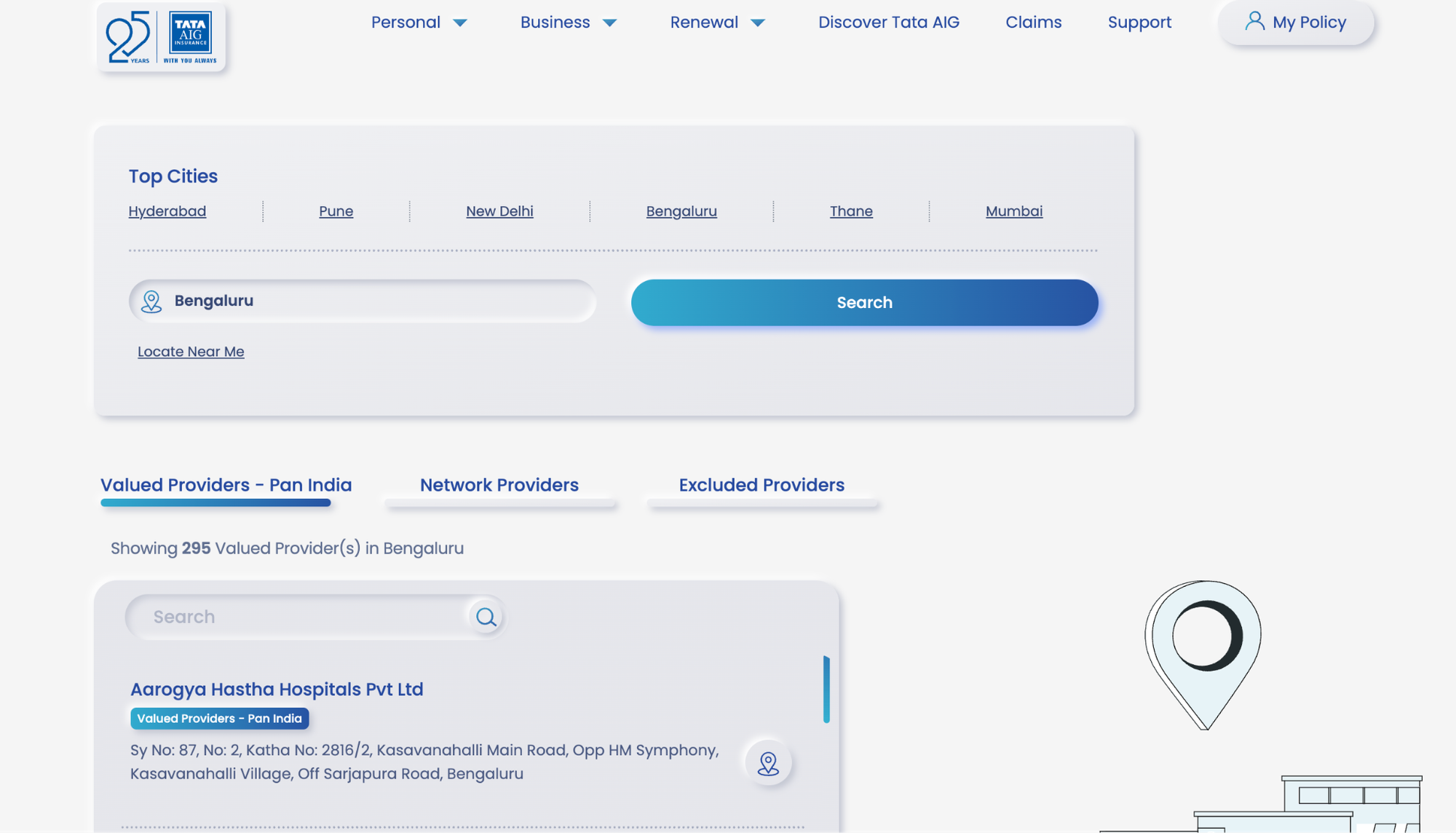
Alternatively, you can check the hospital list in your policy documents or log in to your Tata AIG account via their app on the Play Store and the App Store.
Before we get into hospital types, it helps to understand the two types of claim settlements first.
Types of Claim Settlements
- Cashless Claim Settlement: You are admitted to a network hospital without paying anything upfront. Tata AIG settles the eligible bill directly with the hospital through a Third-Party Administrator (TPA). You may still need to pay non-covered expenses, deductibles, copayments, or charges above policy limits.
- Reimbursement Claim Settlement: You pay the complete hospital bill upfront, collect all original documents, and submit a claim to Tata AIG afterward. The insurer reviews and reimburses the eligible amount, usually within 15-30 days after discharge.
Key Insight
Types of Tata AIG Network Hospitals
- Network Hospitals: Both cashless and reimbursement options are available under network hospitals. Even within the same network, cashless coverage can vary by your policy, room category, and type of treatment, so benefits are not uniform across all hospitals.
- Valued Providers: Certain Tata AIG plans, such as MediCare LITE, operate on a restricted hospital list called the Valued Provider-Pan India network. Cashless treatment is available only at hospitals listed under this network. If you get admitted to a hospital outside the Valued Provider network, a 30% copayment applies to your claim. The only exception to this 30% copayment is hospitalization due to an accident-related injury. We do not recommend choosing a copayment, since the premium discount is disproportionate to the actual 30% out-of-pocket cost you pay.
- Non-Network Hospitals: These hospitals have no tie-up with Tata AIG. Treatment here is not covered on a cashless basis. You'll need to pay the entire bill upfront and apply for reimbursement afterward. That said, under the Cashless Everywhere initiative, you may be able to request cashless treatment even at a non-network hospital in case of an emergency, subject to the insurer's approval. The benefit's applicability still depends on hospital cooperation and insurer coordination.
- Excluded Hospitals: These are hospitals that have attempted to defraud the insurer in the past. Treatment in such hospitals is allowed only in case of emergencies and until the person is stable. You can check the list of blacklisted hospitals on the official website, which is updated periodically.
Now that we know the types of hospitals, let’s understand how the claim process works.
How to File a Claim at Tata AIG Network Hospitals
Cashless Claims
Step 1: Visit the TPA desk at a Tata AIG network hospital. For planned treatment, inform at least 48 hours before admission. For emergencies, inform Tata AIG within 24 hours of admission.
Step 2: Share your Tata AIG health card or policy number, a valid photo ID (Aadhaar or PAN), and any relevant medical records.
Step 3: The hospital submits a pre-authorization request to Tata AIG's TPA on your behalf.
Step 4: Tata AIG/ TPA reviews the request and, if approved, sends a confirmation letter to the hospital. This authorization letter is valid for 7 days from the date of issuance.
Step 5: Proceed with the treatment. At discharge, review and sign all invoices and documents.
Step 6: Tata AIG settles the approved bill directly with the hospital. You pay only for items or services not covered under your policy.
Insight
Reimbursement Claims
Step 1: Get admitted to any hospital and complete your treatment.
Step 2: Pay the full hospital bill at discharge.
Step 3: Collect all original documents, including the discharge summary, invoices, prescriptions, diagnostic reports, and payment receipts.
Step 4: Submit the documents, along with the completed reimbursement claim form, to Tata AIG via their website or by post within the stipulated time.
Step 5: Tata AIG or your TPA reviews your submission and processes the reimbursement in accordance with your policy terms, typically within 21 days.
Why Choose Ditto for Health Insurance?
At Ditto, we’ve assisted over 8,00,000 customers with choosing the right insurance policy. Why customers like Pallavi below love us:

- No-Spam & No Salesmen
- Rated 4.9/5 on Google Reviews by 15,000+ happy customers
- Backed by Zerodha
- Dedicated Claim Support Team
- 100% Free Consultation
Confused about the right insurance? Speak to Ditto’s certified advisors for free, unbiased guidance. Book your call now or chat with our advisors on WhatsApp.
Conclusion
The Tata AIG network hospital list is available on the insurer's official hospital locator and can also be accessed through their app for quick reference.
However, the real value lies in choosing cashless treatment at quality hospitals near you, rather than just looking at the size of the network. If your plan falls under the Valued Provider - Pan India network, such as MediCare LITE, make sure to check the separate list, as the standard network does not apply to you. Before selecting any plan, verify that good hospitals are available in your area and review the policy terms carefully. This helps you avoid surprises and ensures a smoother, stress-free claim experience when you need it most.
If you are looking for more health insurers with 10,000+ network hospitals, explore our guide on the best health insurance companies in India.
Frequently Asked Questions
Last updated on:










