Overview
Most people buy health insurance and never check the hospital list. Then an emergency strikes, and the nearest hospital doesn’t accept their policy. Suddenly, they’re paying out of pocket and filing for reimbursement, which is exactly what insurance is supposed to help you avoid.
This is where the Care Health Insurance cashless hospital list becomes useful. It helps you check which hospitals can offer cashless treatment before you plan admission or face an emergency. Instead of paying out of pocket and chasing reimbursements for weeks, you can have eligible bills settled directly, subject to policy terms.
Free Care Health Insurance Hospital List PDF Download
We've compiled the full Care Health Insurance network hospital list PDF for your convenience. You can find it below:
Note: Hospital lists are constantly changing, and facilities can be added to or removed at any time. Always cross-check with the official locator before planning a treatment.
How to Find the Care Health Insurance Hospital List Online
The most accurate and up-to-date source is the official Care Health Insurance hospital locator on their website.
Step 1: Visit the official website of Care Health Insurance.
Step 2: When you scroll down to the network locator, a pop-up shows up asking if you’re a bank customer or a retail customer.
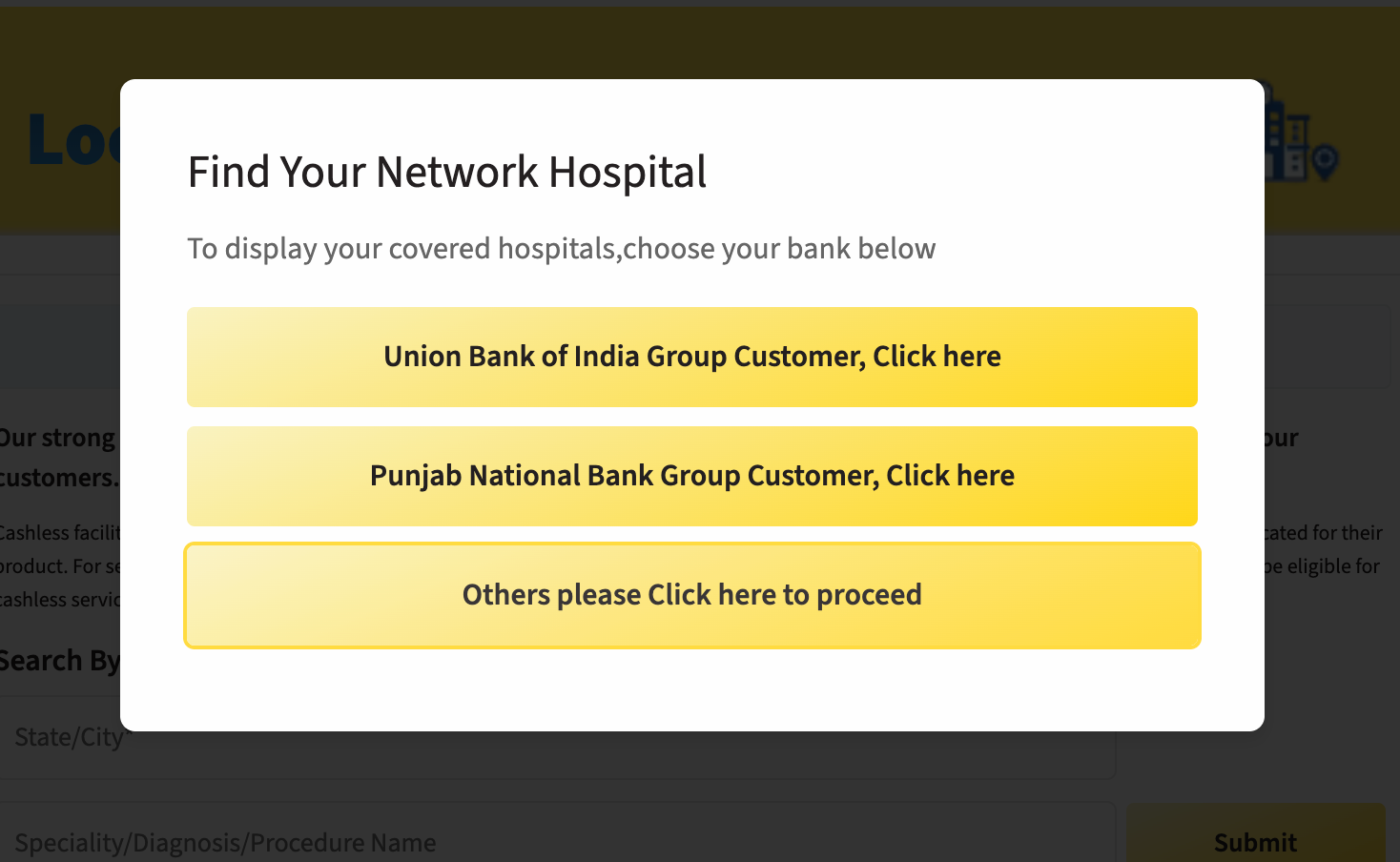
Step 3: Select “others,” then search for cashless network hospitals in your area by state or city, or by the treatment you need.

Types of Care Health Insurance Hospitals
- Network Hospitals
Both cashless and reimbursement options are available in network hospitals. These facilities have an active tie-up with Care Health Insurance. You can walk in, show your health card or policy number, and Care settles the approved bill directly with the hospital. You do not need to pay upfront for covered expenses.
- Smart Select Hospitals
If you choose the Smart Select optional add-on, you get a reduction on your total policy premium. This means if you are treated at a hospital outside the Smart Select list, you bear a 20% copayment on that claim, in addition to any other copayment already applicable to your policy. Stick to the hospitals on the Smart Select list, and no additional copayment applies.
- Surgical-Only Hospitals
Care Health Insurance has specialized surgical-network hospitals that focus on specific procedures, such as ophthalmology, orthopedics, or oncology, rather than general or emergency care. For example, in Bengaluru, hospitals like Nethradhama Super Specialty Eye Hospital fall into this category. Cashless treatment is available here, but only for the procedures they specialize in.
- GIC Common Empaneled Hospitals
The General Insurance Council (GIC) is building a common empanelment model in which hospitals sign a single agreement with the council and all 32 general and standalone health insurers, rather than separate contracts with each insurer. For you as a patient, this means wider hospital access, standardized package rates, faster cashless approvals, and less confusion over your final bill. It is still being rolled out, but GIC-empaneled hospitals already offer consistent cashless treatment, regardless of your insurer.
- Non-Network Hospitals
If you get treated at a hospital outside the Care network, you pay the bills yourself initially. After discharge, you submit all the documents to the insurer for reimbursement, typically within 15 to 30 days. But a cashless option may be available under the Cashless Everywhere scheme, subject to terms and conditions.
- Blacklisted Hospitals
These are hospitals that have attempted to defraud the insurer in the past. Treatment in such hospitals is allowed only in case of emergencies and until the person is stable. You can check the list of blacklisted hospitals on the official website, which is updated in real time.
Did You Know?
How to File a Claim at Care Health Insurance Hospitals?
Cashless Claims
Step 1: Check the Care Health Insurance cashless hospital list to confirm whether the hospital is part of the network. For planned hospitalizations, inform Care at least 48 hours before admission. For emergencies, inform within 24 hours of getting admitted.
Step 2: At the hospital, head to the insurance help desk. Present your health card along with a valid government ID (Aadhaar or PAN).
Step 3: The insurance desk personnel completes the pre-authorization form and submits it to Care, along with your documents, for approval.
Step 4: Care reviews the request. If any information is missing or incomplete, they will follow up with the hospital directly.
Step 5: Care sends its pre-authorization decision to the hospital based on your policy terms and sum insured. If approved, an authorization letter is issued detailing the sanctioned amount and any specific conditions.
Step 6: After your treatment is complete, the hospital submits the discharge summary and all related documents to Care for final approval.
Step 7: Care assesses the bills against your sum insured and plan terms, then settles the approved amount directly with the hospital. You only pay for expenses not covered under your policy, such as consumables or non-medical items.
Key Insight
Reimbursement Claims
Step 1: Get treated at any recognized hospital and pay the bills yourself.
Step 2: Collect all original documents before leaving the hospital, including bills, the discharge summary, diagnostic reports, and prescriptions.
Step 3: Download the reimbursement claim form from the Care Health Insurance Self-Help Portal or the Care Health app. Fill it out carefully and attach all supporting documents within 15 days of discharge.
Step 4: Care's claims team reviews the submission and processes the reimbursement in accordance with your policy terms.
What if Your Claim Gets Delayed?
Why Choose Ditto for Health Insurance?
At Ditto, we’ve assisted over 8,00,000 customers with choosing the right insurance policy. Why customers like Pallavi below love us:

- No-Spam & No Salesmen
- Rated 4.9/5 on Google Reviews by 15,000+ happy customers
- Backed by Zerodha
- Dedicated Claim Support Team
- 100% Free Consultation
Confused about the right insurance? Speak to Ditto’s certified advisors for free, unbiased guidance. Book your call now or chat with our advisors on WhatsApp.
Conclusion
Care Health Insurance has 11,400+ cashless healthcare providers across India, backed by a claim settlement ratio of 93.13% for FY 2022-25. That's a strong combination.
That said, always prefer cashless claim settlements, and confirm that your preferred hospitals are in the network before buying a plan. If you are considering the Smart Select add-on for a premium discount, make sure the hospitals are actually convenient for you, the 20% copayment on out-of-network treatment will cost you more than what you saved. Before finalizing any policy, look at Care Health Insurance reviews, compare claim support and operational metrics with other insurers, along with customer support and network hospital coverage.
Frequently Asked Questions
Last updated on:










