Quick Overview
When you purchase a health insurance policy, not all medical conditions are covered from day one. This is where the 2 years waiting period in health insurance list becomes important. Certain illnesses and procedures are covered only after the policy has been active for a specified duration.
In this guide, we explore what the 2 years waiting period in health insurance list means, why insurers apply it, and which specific illnesses (SI) fall under this category.
How the 2-Year Waiting Period Works and Why Insurers Apply It
The 2 years waiting period in health insurance list refers to an insurer-defined list of specified diseases or procedures (often called specific illnesses or Excl02) for which coverage is delayed until the policy has been active for 24 consecutive months. According to the Insurance Regulatory and Development Authority of India (IRDAI) guidelines, insurers are allowed to impose a specific waiting period of up to 36 months for listed diseases and treatments (though most plans keep this at 24 months). These are generally “slow growing” ailments or procedures that are not typically emergencies but require planned treatment or surgery.
Customers often misread the policy and assume only pre-existing diseases (PEDs) are restricted, but the 2-year list applies even if the condition develops after buying the policy. For PEDs, a separate waiting period of up to three years may apply, depending on the insurer’s terms. And if a condition or procedure falls under both the specific illnesses waiting period and the pre-existing disease waiting period, the longer of the two waiting periods will be applied.
Insurers mandate 2 years waiting period in health insurance list to prevent anti-selection, where people buy insurance only when they know they’ll need surgery soon. Without this, predictable and high-frequency claims like cataract, kidney stones, hernia, or piles can spike right after purchase. This pushes up the incurred claim ratio (the % of premiums paid out as claims) and, in turn, leads to higher premiums or tighter underwriting restrictions. The waiting period helps keep the risk pool balanced and premiums affordable for long-term policyholders.
Did you know?
Some newer and premium health insurance plans remove the specific illness waiting period altogether (subject to medical underwriting and exceptions) like Acko Platinum plan and Manipal Cigna Sarvah Param. Others offer add-ons to reduce the waiting period from 24 months to 12 months (example: ICICI Lombard Elevate).
Claim Disputes and Diagnosis Wording
Claim disputes can happen based on how the doctor writes your condition in the medical reports, not just for the treatment you had. This usually happens when:
- Doctors use broad or general terms (for example, writing “joint problem” instead of saying it was caused by an injury)
- The insurer treats the case as a listed specific illness, while you see it as a sudden health issue
- Hospital discharge summaries use vague wording that matches conditions on the excluded list
Example from Ditto’s Experience: We have seen multiple cases where claims for conditions like anterior cruciate ligament (ACL) or ligament tears, or prolapsed intervertebral disc (PIVD) / slipped discs, were approved because the injury was caused by an accident. This aligns with the insurance definition of an accident: “a sudden, unforeseen and involuntary event caused by external, visible, and violent means.”
However, claims can be denied if the cause does not align with this definition. For instance, a person who tore a shoulder ligament while doing yoga had their claim rejected because there was no external force involved, and the insurer classified it under the specific illnesses waiting period.
That’s why clear medical records matter. In most cases, what’s written as the final diagnosis and the cause in your hospital papers decides whether your claim is covered during the waiting period.
Why is the 2 Years Waiting Period Important for Policyholders
The 2 years waiting period in health insurance list plays a critical role at the time of purchase because:
- It impacts when you can claim for specific illnesses
- It applies to all policyholders, regardless of medical history (this sets a clear, uniform rule upfront, helping customers plan coverage better)
- It is different from the pre-existing disease waiting period
- It resets only on sum insured enhancement, not during portability
Market Reality Check: Most employer-provided group health insurance policies do not apply this specific illness waiting period. However, when you move from a corporate group policy to an individual retail policy, the waiting period rules of the new policy will apply unless you port your policy with continuity benefits.
Diseases Covered in 2 Years Waiting Period in Health Insurance List
The illnesses listed below are the most commonly standardized conditions across insurers. The exact list may vary slightly from insurer to insurer, as permitted under IRDAI norms.
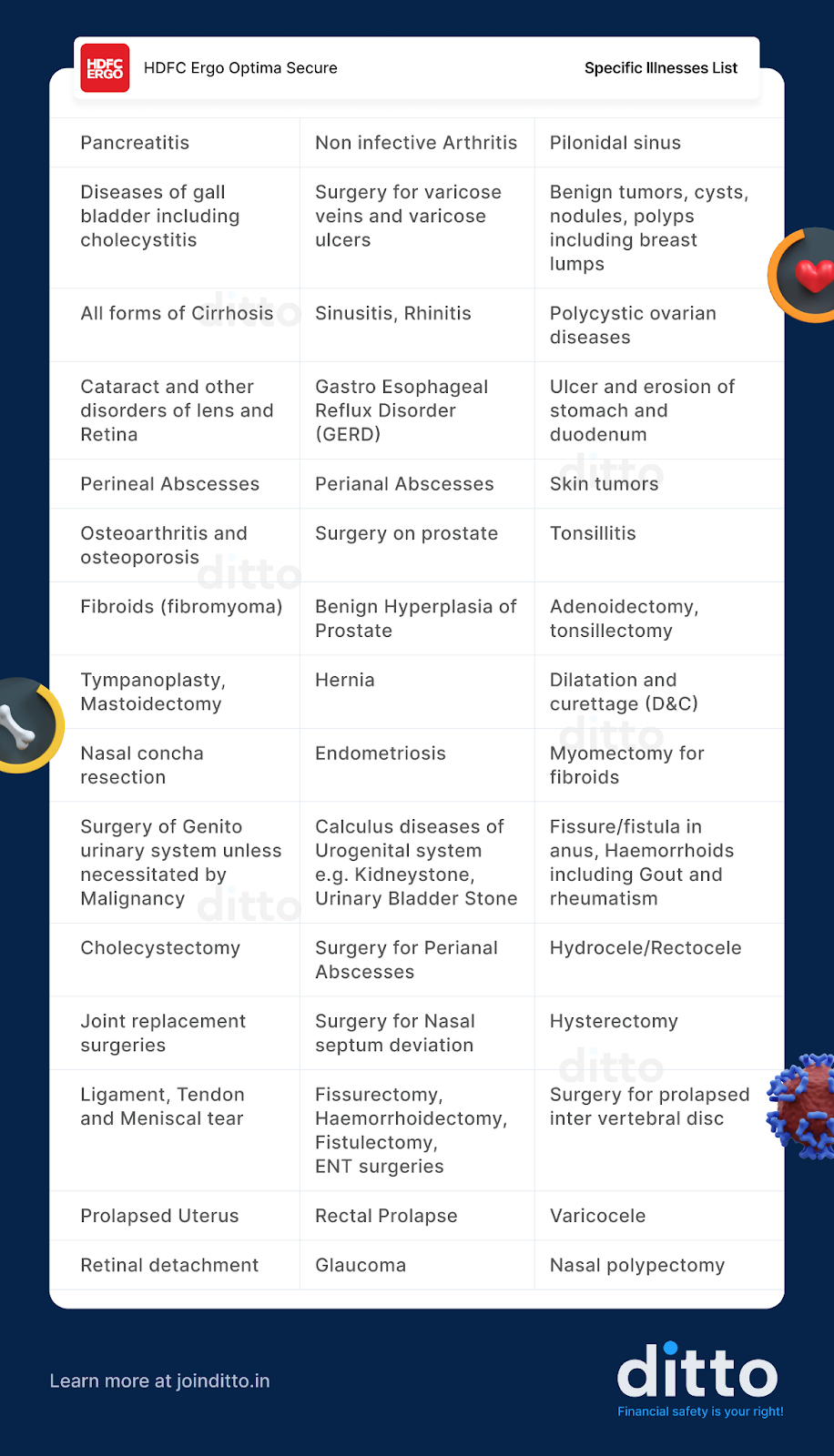
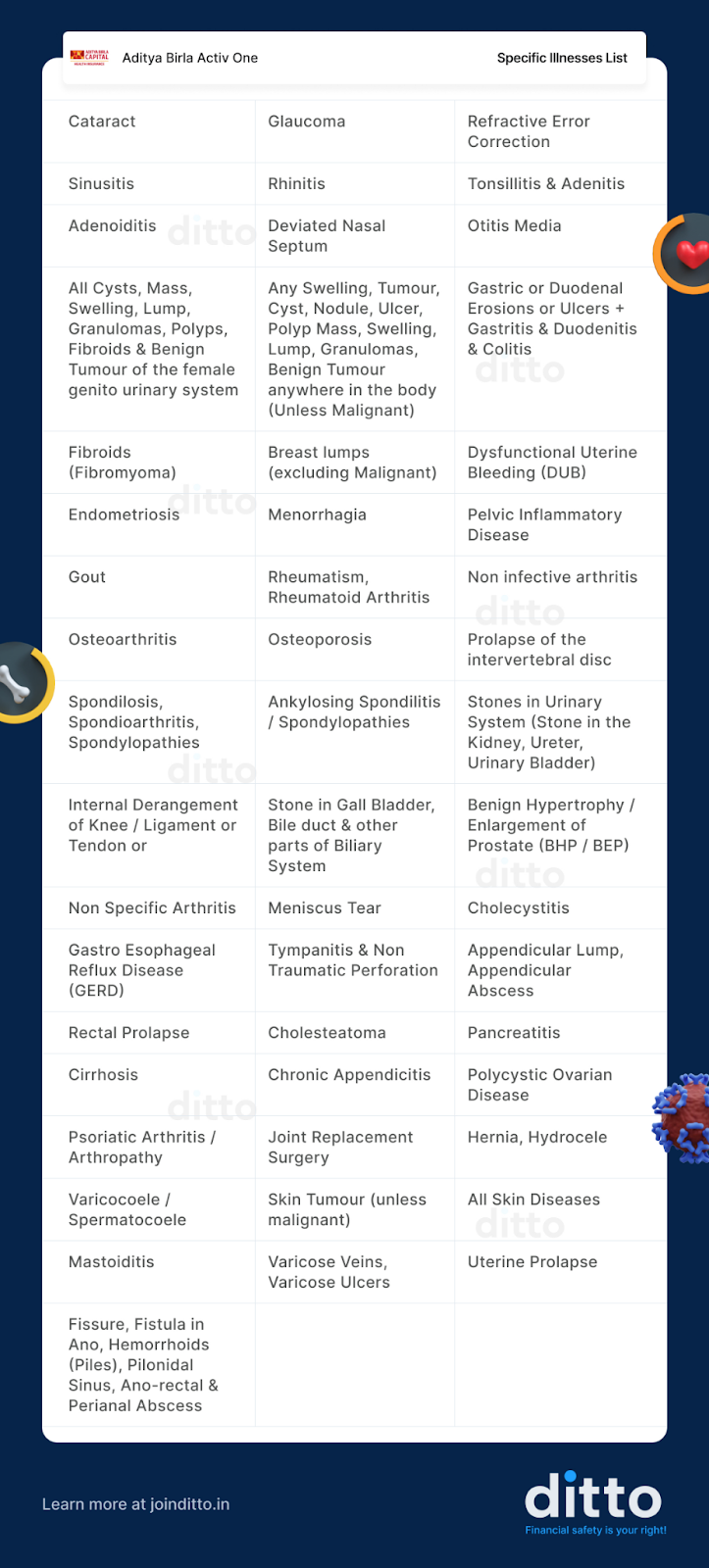
Specific Illnesses Covered Under 2 Years Waiting Period
Surgical Procedures Under the 2 Years Waiting Period
- Hernia (all types)
- Hysterectomy
- Hydrocele / Rectocele
- Joint replacement surgeries
- Cholecystectomy
- Surgery for varicose veins and varicose ulcers
- Surgery for nasal septum deviation
- Fissurectomy, haemorrhoidectomy, fistulectomy
- Myomectomy for fibroids
- Surgery for prolapsed intervertebral disc
- Ligament, tendon, and meniscal tear surgeries
- Adenoidectomy and tonsillectomy
- Tympanoplasty and mastoidectomy
- Dilation and curettage (D&C)
- ENT surgeries
- Surgery on prostate (unless due to malignancy)
These surgeries are not covered in the first two years of your policy, unless they are required due to an accident.
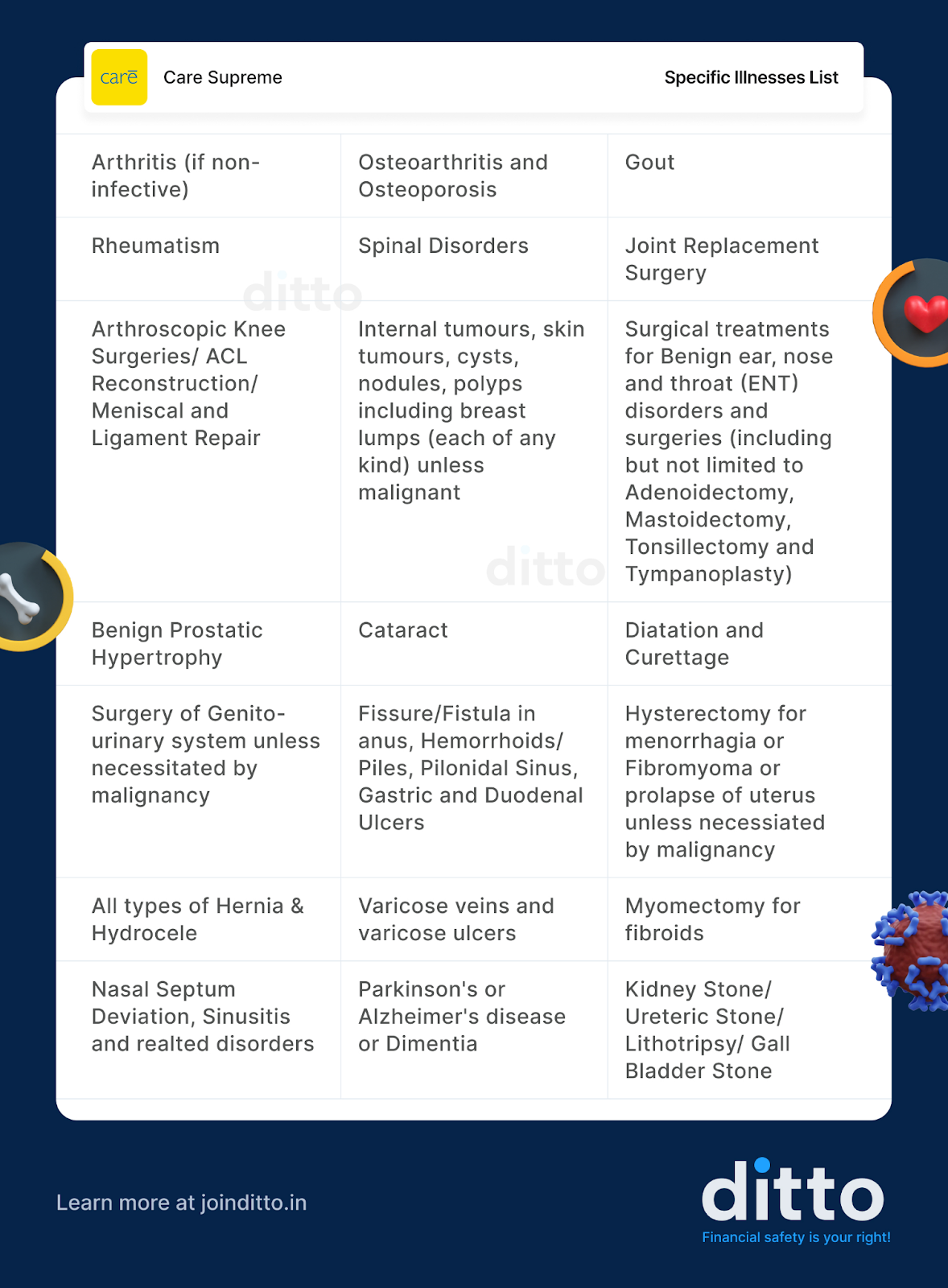

Quick Watch-Out on Specific Illness Waiting Period
- Critical illnesses such as cancer, heart attack, or liver failure are typically life-threatening and cannot be planned, so they are generally not included in the 2-year waiting period for specific illnesses.
- Always check the policy’s SI list carefully. Some plans may still list certain conditions—for example, the Care Freedom Plan from Care Health specifically mentions all types of cancer as a specific illness exclusion for the first 2 years.
Why Approach Ditto for Health Insurance?
At Ditto, we’ve assisted over 8,00,000 customers with choosing the right insurance policy. Why customers like Pallavi below love us:

- No-Spam & No Salesmen
- Rated 4.9/5 on Google Reviews by 15,000+ happy customers
- Backed by Zerodha
- Dedicated Claim Support Team
- 100% Free Consultation
Confused about the right insurance? Speak to Ditto’s certified advisors for free, unbiased guidance. Book your call now or WhatsApp us.
Conclusion
It’s important to review the 2 years waiting period in health insurance list because it helps you understand which illnesses and procedures aren’t covered initially. This way, you can buy insurance early, plan treatments better, and avoid surprise out-of-pocket expenses later. Always review your policy wording and exclusions before purchase to ensure clarity and long-term financial protection.
A quick way to check your policy is to open the policy document and search for “Specified Disease/Procedure waiting period: Code – Excl02,” also referred to as the Named Ailment Waiting Period.
Disclaimer: This article is for informational purposes only. Always consult a qualified insurance advisor before buying a policy and carefully read the policy wording and terms and conditions to understand your coverage.
Frequently Asked Questions
Last updated on:










