Quick Overview
Imagine being discharged after a few tough days in the hospital. The last thing you want is to keep calling customer care to find out where your claim stands. Yet, that’s exactly what happens to thousands of policyholders every year.
Star Health receives claims every day, with 17 crore lives insured since its inception.
In this article, we will discuss how to check your Star Health claim status, download the claim form, and how to avoid common rejection mistakes.
Steps to Track Star Health Insurance Claim Status Online
The quickest way is through the Star Health website. Here’s how:
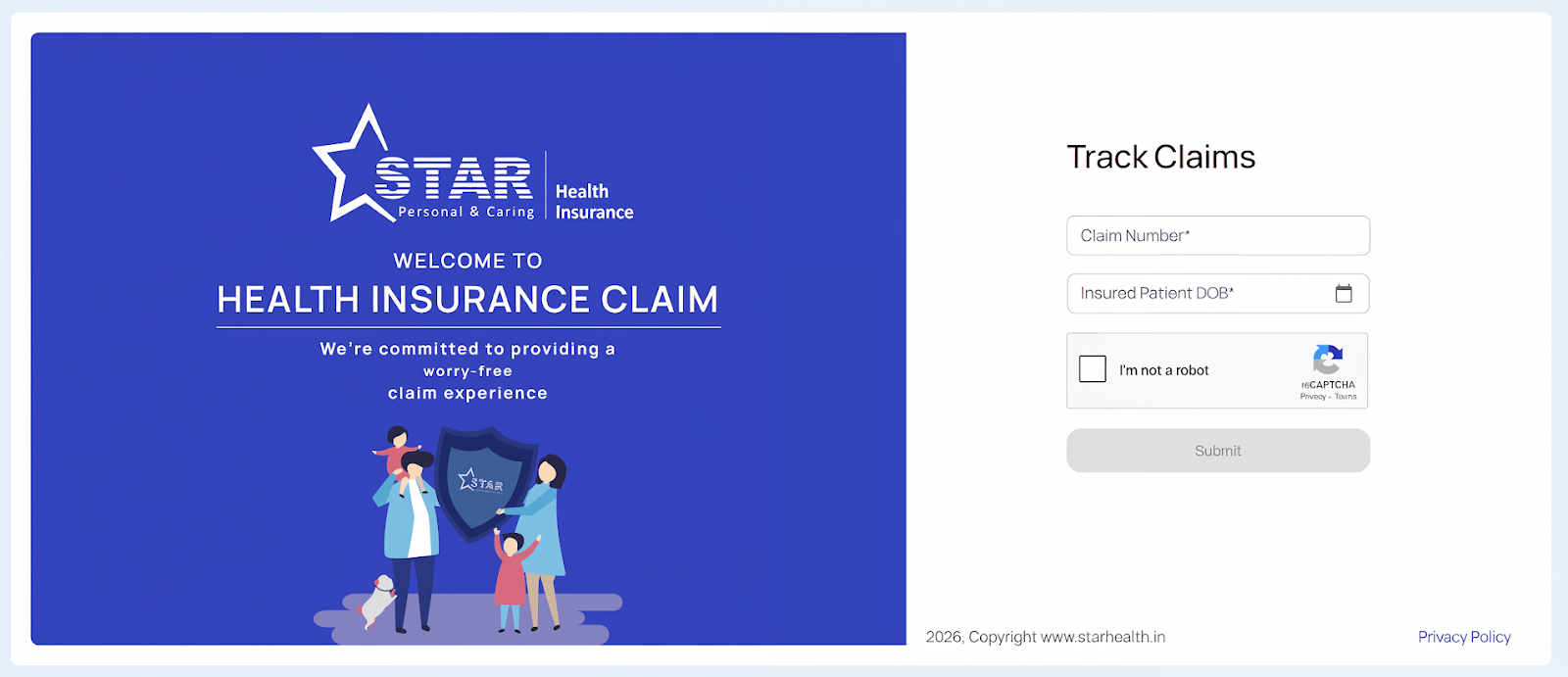
- Enter your Claim Number.
- Enter the Date of Birth of the insured person.
- Fill in the captcha code.
- Click Submit to view your claim status instantly.
You’ll see whether your claim is under review, approved, or if any documents are still pending.
Alternative Ways to Check Claim Status
- WhatsApp: Send “Hi” to 95976 52225 and follow the prompts: Claims > Check Claim Status > Health Policy > enter your Claim Intimation Number.
- Star Health App: Download the app (Android/iOS), log in, and navigate to the “Claims” section.
- Phone: Call 1800 425 2255 (toll-free) to speak to customer care.
- Email: Write to support@starhealth.in with your claim number and policy details.
Did You Know?
How to Download the Star Health Insurance Claim Form
The Star Health claim form comes in two parts, and both must be submitted for reimbursement.
- Part A is filled out by you (the policyholder). It covers your personal information, policy number, hospitalization details, and bank account details for the payout.
- The treating hospital fills out the Part B form. It covers details like the diagnosis, treatment, dates of admission/discharge, and the doctor’s certification.
Steps to Download the Claim Form
- Visit starhealth.in/claims.
- Scroll to the “Download Health Claims Form” section.
- Select the Reimbursement Claim Form (Part A + Part B).
- Download, print, and fill it out carefully.
- Submit along with all supporting documents to Star Health within 15 days of discharge.
Note: You can also pick up the claim form at any Star Health branch or ask the hospital’s insurance help desk for a copy.
Check out the infographic below to learn more about the documents required for a health insurance claim.

Star Health Insurance Claim Settlement Ratio: Why It Matters
The claim settlement ratio (CSR) tells you what percentage of the total number of claims an insurer settled in a given year. A higher ratio implies more claims were honored. Think of it as a ratio to check how reliable your insurer is when it matters.
Source: IRDAI and Star Health’s public disclosures
As you can see, Star Health’s 3-year average CSR is below the industry average of 91.22%.
CSR should be read alongside trends in complaints, claim deductions, service quality, and network usability. Star Health remains the country’s largest standalone health insurer, with an unmatched hospital network of 14,000+ hospitals. But a lower CSR does mean that claims face extra scrutiny. That’s why filing the claim correctly and understanding your policy matters more here than with other insurers.

Common Reasons for Star Health Claim Rejections
Undisclosed Medical History
If you did not disclose a pre-existing condition when buying the policy, related claims may not be paid. Insurers closely review past medical records before approving hospitalization claims.
Documentation Errors
A claim can be rejected for something as basic as missing bills, unsigned forms, or mismatched details. So, before submitting, make sure every document is complete, legible, and consistent.
Network Hospital Rules
Cashless claims usually work best when you get treated at a Star Health network hospital and inform the insurer on time. If you do not, the cashless request may fail, and you may need to claim reimbursement later.
Treatment Not Covered
Not every medical expense is covered under a health insurance policy. If the treatment falls under permanent exclusions, Star Health can reject the claim even if the policy is active.
Check our guide to learn why health insurance claims get rejected.
Why Choose Ditto for Health Insurance?
At Ditto, we’ve assisted over 8,00,000 customers with choosing the right insurance policy. Why customers like Pallavi below love us:

- No-Spam & No Salesmen
- Rated 4.9/5 on Google Reviews by 20,000+ happy customers
- Backed by Zerodha
- Dedicated Claim Support Team
- 100% Free Consultation
Confused about the right insurance? Speak to Ditto’s certified advisors for free, unbiased guidance. Book your call or chat on WhatsApp with us now!
Conclusion
Star Health Insurance offers multiple options for tracking your claim, but that alone does not tell the full story. Given the insurer's lower-than-industry-average CSR and relatively high complaint volume (52 per 10,000 claims), it makes sense to be extra careful with the insurer's documentation and timelines.
Our view: if you are filing a Star Health Insurance claim, double-check everything. Choose a network hospital, submit all documents in one go, respond to queries promptly, and escalate immediately if the insurer misses a promised timeline.
Disclaimer
Frequently Asked Questions
Last updated on:










