Quick Overview
Founded in 2016, Acko started in the general insurance space with a strong focus on motor insurance. It officially entered the health insurance segment in 2020, rolling out plans that were more accessible, digital-first, and customer-friendly. The insurer is one of the top 10 health insurance companies by CSR in India.
Unlike traditional insurers that depend heavily on agents or intermediaries, Acko follows a direct-to-customer (D2C) model. This helps them offer competitively priced, feature-rich policies with a smooth, fully online experience.
In this article, we take a closer look at Acko Health Insurance’s CSR to see whether its claim performance truly matches the reputation it has built over the years.
Acko Health Insurance Claim Settlement Ratio Trends
The figures below are sourced from the insurer’s public disclosures (Form NL 37):
Over the past five years, Acko has maintained a CSR of over 94%, well above Ditto’s recommended 90% threshold. This shows the insurer’s commitment towards providing a great claims experience to its policyholders.
How to Calculate the Acko Health Insurance Claim Settlement Ratio?
Claim Settlement Ratio (CSR), while not the only metric, is one of the most important ways to assess an insurer’s performance. Here’s how it’s calculated:
CSR = (Total no of claims settled / Total no of claims available to settle) X 100Where:
‘Total No of Claims Settled’ includes partly and fully settled claims ‘Total No of claims available to settle’ = (Claims carried forward from the previous year) + (New claims reported) - (Claims closed without payment + Claims still pending at year's end)
Note: The IRDAI doesn’t have any specific formula for calculating the Claim settlement ratio. Hence, these numbers can differ depending on the formula used by different platforms and insurers. We, at Ditto:
- Use the formula mentioned above, as it better captures the actual claim settlement by insurers.
- Recommend looking at the 3-year average CSR, since a single year’s data isn’t enough to judge an insurer’s long-term stability.
- Suggest reviewing the 3-year averages of other key metrics as well, such as average complaints received per 10,000 claims, the Incurred Claims Ratio (ICR) and Gross Written Premium (GWP). This is important because CSR alone doesn’t differentiate between partially and fully settled claims, and cannot give the full picture of an insurer’s performance.
While the Acko claim settlement ratio indicates claim reliability, here are some other important metrics that give a broader view of the insurer’s operational performance.
Other Performance Metrics of Acko Health Insurance
The complaint numbers shown above reflect all of Acko’s products (health, motor, and others), as the insurer does not publish product-wise complaint data separately.
Key Insights
- Average Complaints: Acko sees a three-year average of 19.29 complaints per 10,000 claims, which is on the higher side compared to some of the top insurers (like Bajaj and HDFC ERGO) that usually report below 15. While the complaints figures are decent, this shows there’s still room to enhance post-sale support and claim handling.
- ICR: With an average ICR of 66.20% between FY 2022-25, Acko falls well within the healthy range of 50–80%. This means they’re paying a reasonable share of premiums as claims, while keeping the business sustainable.
- Annual Business: Acko Health Insurance’s annual business, measured by Gross Written Premium (GWP), has grown steadily from ₹736 crores to ₹930 crores over the last three years. This steady rise shows that it is expanding its presence in the health insurance market. However, it still has a long way to go before it reaches the industry average of ₹3,969 crores.
- Network Hospitals: It has a network of 10,000+ hospitals, giving customers access to cashless treatment across different cities and towns. However, policyholders should always check the up-to-date hospital list before undergoing treatment.
Top 10 Health Insurance Providers by Claim Settlement Ratio in 2025
To help you see how Acko Health Insurance stacks up against other leading insurers in terms of claim reliability and efficiency, check out the infographic.
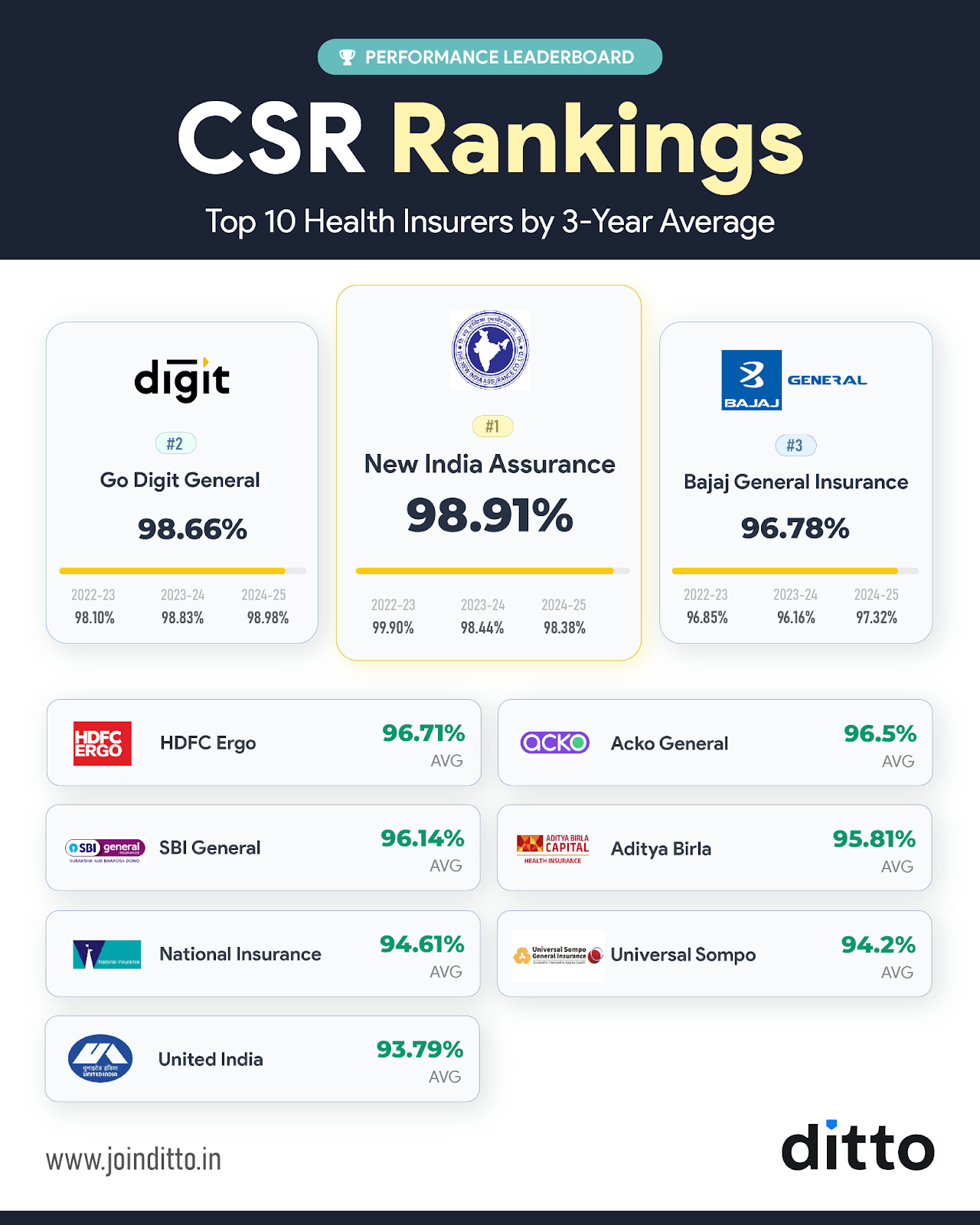
As seen in the infographic, Acko prominently features among the top health insurers by CSR. This suggests that it demonstrates top-notch claims-handling efficiency.
Why Approach Ditto for Health Insurance?
At Ditto, we’ve assisted over 8,00,000 customers with choosing the right insurance policy. Why customers like Pallavi below love us:

- No-Spam & No Salesmen
- Rated 4.9/5 on Google Reviews by 15,000+ happy customers
- Backed by Zerodha
- Dedicated Claim Support Team
- 100% Free Consultation
Confused about the right insurance? Speak to Ditto’s certified advisors for free, unbiased guidance. Book your call or chat with us now, slots fill up fast!
Acko Health Insurance Claim Settlement Ratio (Ditto’s Take)
Acko Health Insurance’s CSR averages around 96.50% (FY 2022-25), indicating reliable claims handling. Its plans are competitively priced with some attractive features. However, the use of TPAs, a no-agent distribution model, and the fact that it is a relatively new health insurer with a limited track record are aspects that require careful consideration.
If you’re considering Acko’s plans, make sure you compare all your options and read the fine print carefully to avoid any surprises in the future.
Note
Frequently Asked Questions
Last updated on:










